An elderly patient presents with worsening vision in one eye over the last 2 days. There is no pain and there has been no trauma.
The patient’s visual acuity is significantly reduced in the affected eye and you question if there is an afferent pupillary defect.
Your differentials here include retinal detachment, so you decide to perform an ultrasound.
How to perform eye POCUS?
Do NOT perform ultrasound on the eye if there is suspicion of a penetrating globe injury
- Use the vascular probe (high frequency linear probe)
- Place a Tagaderm over the shut eye
- Use a lot of gel
- This not only gives a better view, but also decreases the pressure applied on the eye.
- Use the probe to get a good view of the whole eye including the nerve.
What do we expect to see?
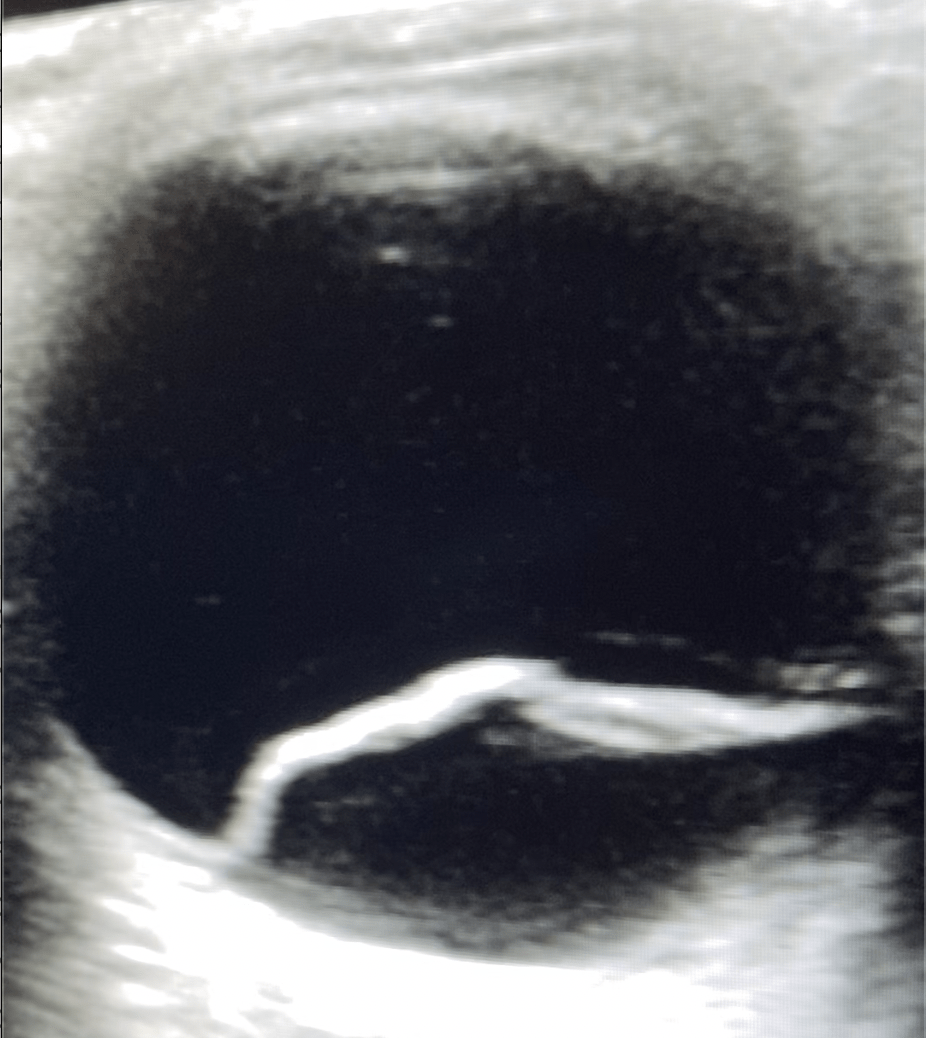
In Retinal Detachment, the hyper echoic line is uniform and doesn’t cross the optic nerve, whereas in vitreous detachment, it does and is usually less uniform due to inflammation and haemorrhage.
What can eye POCUS be used for?
Retinal detachment
Lens Subluxation
Vitreous Haemorrhage
Retinal Detachment vs Vitreous Detachment
A rapid history of the progression of the disease, any relevant past history, including diabetes, is important.
The clinical examination relies as always on the big 3:
- Visual Acuity: It is helpful to know previous acuity also
- Visual Field defects:
- For example, superior retinal detachment results in an inferior visual field defect.
- Pupillary Response including Relative Afferent Pupillary Defect(RAPD)
Note that direct ophthalmoscopy should also be performed, however you may not be able to detect the more peripheral retinal tears or detachments.
Posterior Vitreous Detachment
It occurs when the vitreous degenerates and separates from the retina. It tends to be age related.
Clinically the patient usually presents with:
- Normal Vision
- No visual field defect
- No RAPD
- May have ‘flashes’ that occur due to the vitreous pulling on the retina as it detaches
Retinal Detachment
This can occur following a retinal tear, which allows fluid from the vitreous to enter under the retina, separating it.
Clinically the patient usually presents with:
- Visual field loss
- May describe a curtain coming down over the eye
- RAPD
- Central loss of vision may indicate macular detachment(may not be reversible)
What is the relative afferent pupillary defect(RAFD)?
The RAPD is also called the Marcus-Gunn pupil. It indicates optic nerve or retinal disease. It also requires that the disease be only in one eye ie., bilateral disease may not produce a defect.
It should be performed in a dimly(not dark) lit room, with a strong light source. Swing the light from eye to eye. Shining the light on either pupil should make both pupils constrict. This is the direct and consensual response.
A positive RAPD is diagnosed when the pupil that has the light directed at it, does not constrict, but dilates.
What are the causes of RAPD?
- Optic Nerve Damage
- Trauma
- Ischaemia
- Tumour
- Glaucoma
- Ischaemic disease of the retina
- Retinal detachment
- Severe unilateral macular degeneration
- Intra-ocular tumors
- Retinal infections
These are only some of the causes. Think of anything that causes optic nerve or retinal damage.
References
- Lahham S, et al. Point-of-care ultrasonography in the diagnosis of retinal detachment, vitreous hemorrhage, and vitreous detachment in the emergency department. JAMA Netw Open. 2019;2(4):e192162.
- Johnson D, Hollands H. Acute-onset floaters and flashes. CMAJ 2012;184:431.










As an entrepreneur, your customers and your team rely on you to deliver. Try to harness your team’s energy towards your vision and do everything you can to avoid being distracted. A lot of businesses fail once the vision becomes blurry.”
this blog is great for our country to be a valuable blog and would like to visit you
visit my site for sure and you will not be good for the good thank you and have a nice day
카지노사이트
everyone who wants to pursue life try to visit the site to and you will not regret
this is the day that all I thought was correct was wrong but when I visited the site I was not in the side because of the usual example I learned
do not forget that you do not care about the problem the guy does not wanna let them make love to you so that visitor to the site to and you do not repent
바카라사이트