Introduction
A 38 year old woman presents to the emergency department, with sudden onset severe headache, which she describes as being “hit on the head with a shovel’. She is not a headache sufferer and has no other past medical history. Her conscious state is normal and the headache has subsided. We suspect a sentinel bleed, or warning leak headache and want to rule out subarachnoid haemorrhage(SAH). How should we investigate this patient?….or should I say how do we actually investigate?
It seems that if you ask a handful of doctors, be they Emergency Physician or Neurosurgeons, you get a handful of different responses. There doesn’t seem to be a great deal of consensus. Should there be? Is the evidence such, that we should all be doing one thing?
The traditional approach is to perform a non-contrast CT brain and follow with a lumbar puncture(LP) if this is normal. This traditional thinking has been interrupted, since recent studies looking at early CT ruling out SAH. The timing and way we interpret our lumbar punctures has also changed. The gold standard of xanthochromia, has been weakened by the understandable need to perform taps at less than 12 hours, post headache onset. There has also been the movement away from xanthochromia testing, due to the lack of availability of spectrophotometry, towards the use of a red blood cell cut off points, or even visual confirmation of cerebrospinal fluid(CSF) discolouration. There has also been the recent discussion about a greater use of CT Angiography(CTA).
Survey Results
I recently sent out a survey on SAH diagnosis, on this site and chose the first 100 responses to the questions asked. In this blog, I wanted to use those responses to answer three questions:
- Can we rule out out subarachnoid haemorrhage with early CT?
- What is the role of lumbar puncture and how should we perform it?
- Where does CTA fit into all this?
Here are the Questionnaire Results
In the questionnaire I made the following statement relating to a GCS 15 patient with sudden headache and no neurology:
If a patient presented within 6 hours of headache onset and the CT Brain shows no blood- I’m Done
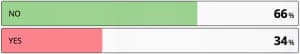 Only one third of physicians would accept a negative CT as ruling out subarachnoid haemorrhage if done within 6 hours of headache onset.
Only one third of physicians would accept a negative CT as ruling out subarachnoid haemorrhage if done within 6 hours of headache onset.
Of those that would perform further testing 60% would perform a lumbar puncture. The remainder would perform a mixture of LP and CTA

If they did perform a LP 61% waited for 10-12 hours i.e. 39% did not.
 ….and only 31% used spectrophotometry
….and only 31% used spectrophotometry
‘If a patient with sudden headache onset has a normal CT brain I would perform a CTA rather than a lumbar puncture. If the CTA were negative, I’m done, If positive I would then perform an LP?
 31% would adopt this approach. Now the question was leading and the answer may be confounded by the fact that it’s what I have discussed and presented at the EMCORE Conference last year, This may be utilised more, in the rural sector, where LP results can be 24 hours plus away.
31% would adopt this approach. Now the question was leading and the answer may be confounded by the fact that it’s what I have discussed and presented at the EMCORE Conference last year, This may be utilised more, in the rural sector, where LP results can be 24 hours plus away.
Let’s Look at The Evidence
Here are the facts:
SAH occurs in about 1/10,000 of the population i.e. < 0.001%
Only 10% of patients who present with sudden onset of headache, will actually have a Subarachnoid Haemorrhage.
10-15% will die at the time of the bleed. If it is a warning leak headache and the patient presents with nothing more than a headache and they re-bleed, 50% will die. Of those remaining only half will go back to a normal functioning state.
This is why we get scared of it. Why do we need to get a diagnosis quickly? Because 15% of the well patients will have a re-bleed in the first few hours. The majority of these patients don’t do well. Almost half will have a re-bleed in the first 4 weeks after a sentinel bleed.
Can CT within 6 Hours Rule Out SAH?
There is only one prospective study in this area, all the rest are retrospective.
In 2011 Perry et al(1) conducted a prospective multicentred cohort study with over 3000 patients. 953 patients had a CT in < 6 hours. 119 of these were diagnosed with a SAH. Of the remaining 834 patients with a normal CT at 6 hours, no patients died, although a number of patients were lost to followup.The conclusion was that with a 3rd generation scanner and if performed within 6 hours of headache onset, the CT scan had a 100% sensitivity. This was a welcomed finding, in a study with some issues, on which I wrote a review at the time. The concerns with the study were:
- There was no gold standard- being alive at 6 months was the parameter used. This doesn’t exclude an aneurysm, however given that most patients with a bleed have a catastrophic re-bleed within a month, its probably good enough.
- Not all patients had a lumbar puncture performed.
- 13 patients in the CT in < 6 hours group, were lost to followup.
- The 95% confidence intervals were 97%-100%
In 2012 Backes et al(2) conducted a retrospective study looking at this same question. In this study all patients who had a CT had an LP. Of 137 patients who had a CT brain in < 6 hours, 68 were diagnosed with a SAH.Of the 69 patients with a normal CT, CSF was only positive in one and this was due to a cervical AV malformation. The sensitivity was 98.5% with 95% confidence intervals of 92.1-100%
In 2015 Blok et al (3) again addressed the question in a retrospective study and found a negative predictive value of a CT done within 6 hours as being 99.9%. This study had some limitations.
So a CT within 6 Hours of Headache onset is GOOD, its GREAT, But is it good enough to rule out the SAH? Are you done? Finished? Go home?
NO, we cannot definitely rule out SAH with CT in < 6 hours.
A CT scan at < 6 hours cannot rule out SAH, with 100% assurance. This is a condition with such potentially devastating consequences. The standard of care is non-contrast CT brain, which if normal is followed by an LP looking for xanthochromia.
One of my greatest concerns in respect to CT ruling out SAH is in respect to who reads it and the chance of error. I have a low resolution screen in the emergency department in which I work. I view X-rays on this and sometimes CT’s but the quality is awful. My biggest concern is not that I’ll miss it, but that the radiologist, especially the after hours guy reading it from somewhere else, may miss it. It’s happened.
Shared Decision Making.
This may be where shared decision making comes into the picture. I know a lot of you are doing it. You explain to the patient that the risk of missing it according to the studies is at best 0% and at most 3%. Given that about 10% of all sudden headaches in well patients are due to aneurysms, the risk is about 3 in 1000 or simply about 1 in 300.
In a retrospective observation study by Sayer et al(6) where an LP was performed following a negative CT brain, of 1898 patients having an LP there were 92 positives, of which there were only 8 aneurysms. This is a sensitivity of about 0.4%. Similar to above.
You also explain the potential issues with lumbar puncture:
- It’s a blind test and although ultrasound can be used, in most cases it is performed by feel.
- The procedure is operator dependant, but even the most experienced can sometimes miss it.
- There is a risk of needlestick injury
- The risk of post-LP headache is almost 40%(5)
- There is a risk of introducing infection
I’m always a little concerned about shared decision making, as I believe we can influence what the patient’s response will be, not making it shared, but biased.
What About Lumbar Puncture?
The accepted rule-out of SAH in the GCS 15 patient who has presented with a sudden onset severe headache is CT without contrast followed by LP at 12 hours testing for xanthochromia. Let’s consider that SAH is the only diagnosis here i.e., meningitis is not a possibility, although this too can present with sudden onset headache, but will have other symptoms associated with it.
The next statement made was; ” When I perform an LP I only do so after 10-12 hours” The answers were:
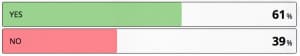 Less than half of responders did this. The question that needs to be asked is: Do they have access to spectrophotometry? If not, they may not see a reason to wait.
Less than half of responders did this. The question that needs to be asked is: Do they have access to spectrophotometry? If not, they may not see a reason to wait.
If I perform a lumbar puncture I only use spectrophotometry
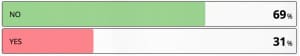

Only one third use spectrophotometry.
A lumbar puncture performed too early i.e.., within 2 hours of headache, may miss a SAH, as red cells have not had time to track down the spinal canal. Do you test for numbers of red blood cells? There have been cut off points recommended, for diagnosing SAH. The problem with red cell counting is that we cannot predict which taps are traumatic(7). We know that clearing of red cells between the first and fourth tube doesn’t help us as this can also happen in SAH.
Xanthochromia is essential to making the diagnosis in SAH. Although false positives can occur, it is the gold standard in CSF analysis. The breakdown of red cells into bilirubin can only occur in vivo. This can take up to 12 hours to develop(8), where its sensitivity is 100%. If you are performing an LP at 12 hours and testing for xanthochromia, it gives you the best sensitivity. If the LP is performed at less than 12 hours post headache, there is a chance of missing some patients with SAH.
What about those cases where you will not get a xanthochromic result back for 24 hours. In rural centres, if the last flight of the day, usually late afternoon at the latest is missed, then the test is not performed until the next day. There is a problem in this group, as you cannot get a definite answer. Perhaps this is where CT Angiography(CTA) can help.
Is there a role for CTA?
There is not a lot of evidence for CTA in the rule out stage. In 2016 at EMCORE we presented a study which looked at the use of CTA(9). This was a mathematical model, as an adequately powered study would need some 3000 patients enrolled. This model concluded that a negative CT brain and a negative CTA has a post test probability of excluding a SAH of 99.43%.
In most cases, when a CT and/or LP are positive, the Neurosurgical team ask for a CTA.
There are some issues with a CTA:
- Aneurysms may be missed, especially if small
- There is the exposure to ionising radiation and the use of contrast medium.
- The aneurysm may be in spasm and just doesn’t appear. This sometimes occurs when Neurosurgery perform Digital Subtraction Angiography. Their approach to this is to bring the patient back in two weeks and repeat.
- What if you find an aneurysm? We know that the rate of aneurysms found incidentally in the population is around 2%. Is that aneurysm responsible for the headache, or is it due to another cause?
I look at the role of CTA a little differently. I find it very useful if I’m in a situation where I won’t get my CSF results back until next day, as they have to be flown to a major centre. I will perform the CT and then the CTA. If positive, I refer to Neurosurgery.
I discuss the CTA investigation with patients after a normal CT brain. I discuss the radiation and contrast risks as compared to the discomfort and potential false negatives/positives of LP, or not being able to get an LP answer.
I consider the CTA after the CT. If positive, I really need to find out if the aneurysm has been one that’s bled, so I perform an LP, following discussion with the patient.
Let’s also remember that the cause of a sudden severe headache is not binary i.e., it’s not simply SAH or not. There are many other potential causes. Some are benign such as sinusitis, or migraines, whereas others may be more sinister and include meningitis and encephalitis, where an LP can assist in the diagnosis. There are also cases where the CTA may assist. These include:
- Arteriovenous Malformations
- Cerebral Venous Thrombosis
- Dissection of the Carotid/Vertebrobasilar arteries
Magnetic Resonance Angiography(MRA) vs CTA
Should these patients be getting MRAs? Firstly there is the limited accessibility to MRA. Although the Magnetic Resonance Imaging is available in larger centres it is not readily accessible. There is the benefit of no radiation exposure and no use of contrast, versus the issue of delay. In terms of the information given, the CTA with newer multi-slice scanners is at least equivalent and preferred in the acute setting(10,11).
Conclusion
So where are we with all this? Our CT scanners are getting better and better and we will reach a time where they can rule out subarachnoid. Right now they can’t, although when performed at <6 hours after headache onset, they come close.
The condition itself is potentially catastrophic and any shared decision making needs to convey that to the patient, so they truly are informed. However to rule it out today, we need an LP following a negative CT and that LP needs to be done at 12 hours, to ensure xanthochromia is present.
The role of CTA? I believe there is one.
My personal approach(and this is my approach), to the well patient with no neurology, where I’m concerned about SAH, is
- Perform the non-contrast CT
- If done < 6hours from headache onset and is normal, I will discuss with the patient and explain the risks and the lower chance of a SAH being present
- If done > than 6 hours from headache onset, I explain the lower sensitivity of the scan
- I will usually recommend an LP, which will be tested for xanthochromia. I consider this a simple test, one that I’ve performed many times and although there are some risks, they are small. The added benefit of the LP, is that it allows me to make other diagnoses that may have caused the headache.
- If the patient doesn’t wish to have an LP, or if I’m considering another vascular cause of headache, I will offer the patient a CTA, with the associated explanation of radiation exposure and contrast use.
- If I’m in a centre where the lumbar puncture results may not come back until the next day or if there is no xanthochromic testing, I offer a CTA.
- If the patient refuses the LP and CTA, or if a CTA can’t be done, due to significant renal impairment, I consider booking an MRA
- Do I discuss this with Neurosurgery? If I’ve done a CT and LP with Xanthochromic testing and all is normal, no I don’t. Remember we are dealing with a GCS 15 patient with no neurology. In other cases, I often do.
There are so many possibilities as well as alternative diagnoses, as well as limitations that it makes this a difficult area.
Let me know what you do, and the potential approaches out there.
References
- Perry, Stiell et al., Sensitivity of computed tomography performed within six hours of onset of headache for diagnosis of subarachnoid haemorrhage: prospective cohort study. BMJ 2011;343:d4277
- Backes D et al. Time-Dependent Test Characteristics of Head Computed Tomography in Patients Suspected of Nontraumatic Subarachnoid Hemorrhage. Stroke. 2012;43:2115-2119
- Blok KM et al., CT within 6 hours of headache onset to rule out subarachnoid hemorrhage in nonacademic hospitals. Neurology. 2015 May 12;84(19):1927-32
- Perry J, Spacek A, Forbes M, et al. Is the Combination of negative computed tomography result and negative lumbar puncture result sufficient to rule out subarachnoid hemorrhage? Ann Emerg Med 2008;51:707–13
- Kuntz K, Kokmen E, Stevens J, et al. Post Lumbar puncture headaches: experience in 501 consecutive procedures. Neurology 1992;42:1884–7.
-
Sayer, D et al. An Observational Study of 2,248 Patients Presenting With Headache, Suggestive of Subarachnoid Hemorrhage, Who Received Lumbar Punctures Following Normal Computed Tomography of the Head. Journal of Academic Emergency Medicine. 2015 Nov; 22(11):1267-73
-
Buruma OJ, Janson HL, Den Bergh FA, Bots GT. Blood-stained cerebrospinal fluid: traumatic puncture or haemorrhage? J Neurol Neurosurg Psychiatry 1981;44:144–147
- Vermeulen M, Hasan D, Blijenberg BG, Hijdra A, van Gijn J. Xanthochromia after subarachnoid haemorrhage needs no revisitation. J Neurol Neurosurg Psychiatry 1989;52:826–828
- McCormack RF, Hutson A. Can computed tomography angiography of the brain replace lumbar puncture in the evaluation of acute-onset headache after a negative noncontrast cranial computed tomography scan?. Acad Emerg Med. 2010 Apr;17(4):444-51
- Gihan Hassan Gamal. Diagnostic accuracy of contrast enhancement MRI versus CTA in diagnosis of intracranial aneurysm in patients with non-traumatic subarachnoid hemorrhage. The Egyptian Journal of Radiology and Nuclear Medicine
Volume 46, Issue 1, March 2015, Pages 125–130 - Yoon et al. Imaging of cerebral aneurysms: a clinical perspective. Neurovascular Imaging 20162:6











My decision rule is similar but modified by working in a centre with a high rate of obesity, 72% of our population are overweight or obese including 12% who are morbidly obese.
So I will either go CT /LP if I anticipate and LP being achievable or if an LP is very likely to be really difficult then I’ll go CT /CTA. Likewise if the patient will not consider an LP then I’ll go CT/CTA straight up
A good point. Some patients are not that overweight, but seem to have a large fat pad in the lower back.
There is no Consensus in the way we investigate potential subarachnoid haemorrhage! – Resus
[url=http://www.g551q7dj57l3144supja746h5dtk93vls.org/]ugtldihwti[/url]
agtldihwti
gtldihwti http://www.g551q7dj57l3144supja746h5dtk93vls.org/
ブランドコピー代引き
Double-Position Vertical Vibration Concrete Pipe
ブランドバッグコピー
Pro Audio Power Amplifier
Mini Gas Lantern
スーパーコピーブランド
Ems Abdomen Patch Series
ブランド時計コピー
Cnc Milling Factory
ブランドバッグコピー
スーパーコピーバッグ
All In One Screen
ブランドスマホケースコピー
Flush Wipes
Cartierカルティエ時計コピー
Pcb Control Board
mobile toilet trailer for sale
ブランド時計コピー
ブランドMCMエムシーエム財布コピーN級品
China Plastic Oil/ Water Drum Blow Molding Making Machine /Make Machinery
Fendiフェンディバッグコピー
China Coverall
ブランドPradaプラダバッグコピー代引き
1325 Wood Router Machine
Air Conditioning System For Agriculture Vehicle
ブランド財布コピー
ブランドGucciグッチネックレスコピーN級品
Double Toggle Switch
Fendiフェンディ帽子スーパーコピー
Injection Moulding Tool Design
ブランドコピーBalenciagaバレンシアガN級品
Funke Plate Heat Exchanger
Goyardゴヤールスーパーコピー
TECH-BIO Hand Sanitizer Scented 50 ML
スーパーコピーバッグ
7 Gauge Taper
2 Galvanized Fence Pipe
10.1 Inch SC9832 CPU Android 4G LTE Tablet PC
ブランド財布コピー
Solar Power System Grid Connected
30208
最新ブランドスーパーコピー代引き