1. History and Rate
HISTORY
The story is so important to get early. Why? Because it primes us for how to look at the ECG.
Always ask, “What has the patient presented with?”
If the answer is chest pain, then we can zero in on looking at ischaemic changes in the appropriate arterial territories, i.e.., inferior, anterior and lateral. We’ll look for ST elevation or depression and reciprocal changes.
If the answer is palpitations, then we look at the rhythm strip, lead II and pay attention to the rate, as it’s the tachycardias that result in palpitations. We can look for changes that may be consistent with arrhythmias i.e., Brugada, Wolff-Parkinson-White, epsilon waves etc.
It is possible to get ischaemia, leading to ventricular tachycardia and palpitations.
Password is ‘ecg’
RATE
An ECG is produced in 10 seconds. Pay attention to the calibration.
It should be 1mV = 10mm and 25mm/sec.
My preference for calculating the rate is simply to measure the number of QRS complexes in the full run of the rhythm strip and multiply by 6. This gives number of complexes in 60 seconds.
Try these examples
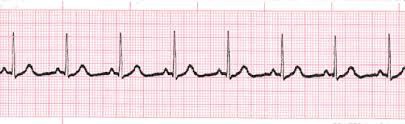
Look at the above ECG and count the rate
2 large squares between RR= 150bpm
3 large squares between RR = 100bpm
4 large squares between RR = 75bpm
5 large squares between RR = 60bpm etc..
Both atrial and Ventricular rates are at 75bpm.
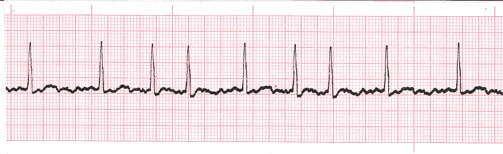
What is the rate in the rhythm strip above?
This is an example of atrial fibrillation. Because the rate varies, it may be difficult to use the large squares approach. I count the number of QRS complexes across the whole length of the ECG and multiply by 60, to give the number of ventricular complexes i.e.., beats per minute.In this ECG there are 8 complexes. This makes the rate 6 x 8 = 48bpm.
Below is another example. What is the rate?
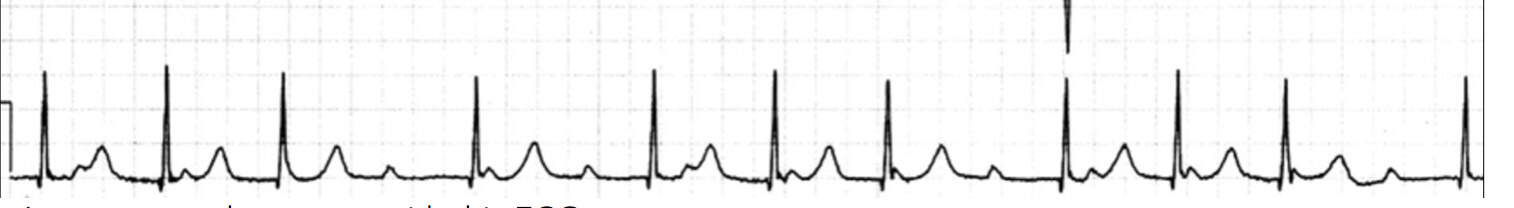
Remember to calculate an atrial and ventricular rate
Calculate the atrial and ventricular rate in the strip above.
The ventricular rate is 11 QRS complexes x 6 = 66/minThe atrial rate appears to be 13 p waves x 6 = 78 complexes/min
When there are more P waves than QRS’s, think of AV dissociation/ Mobitz Blocks. (More on this in the next section).
If the QRS numbers are greater than the p waves, then there may be a accelerated AV rhythm occurring.









