A 28 year old woman presents to the emergency department with one week of headaches. The headache is worst on waking and improves during the day. It’s worst if she coughs and bends. Today she has awoken with a headache and right eye pain.
The patient has a past medical history of migraines, however these headaches, even the one she has today are different. On systems review, the only other history is a weight gain of 15kg during COVID lockdown.
Examination demonstrates dual heart sounds, clear chest and soft abdomen. Neurological examination is normal although fundoscopy is difficult to perform.
This patients’s history shows evidence of raised intracranial pressure ie., the morning headache that improves during the day and the increase in headache that occurs with movement and coughing. This patient needs a workup and may will need referral to neurology and/or a neuro-ophthalmology service.
Idiopathic Intracranial Hypertension
Idiopathic intracranial hypertension(Primary pseudotumour cerebri syndrome (PTCS)) is raised intracranial pressure of unknown cause. It is called pseudotumour cerebri, because the symptoms mimic a tumour, without one being present.
There is an association with patients who are obese, but it is also shown to occur in patients who are not obese, but have had a weight gain of more than 5%.
It tends to occur in female patients of reproductive age. Over 90% of patients are overweight. The association with obesity or weight gain in male patients is less clear, with only about 25% of males with the same condition being overweight.
Symptoms
Symptoms include the following:
- Headache
- Nausea +/- vomiting
- Transient visual loss, although permanent visual loss can occur
- Patients with a BMI > 40 kg/sqm are more likely to present with severe papilloedema and trend towards more severe visual loss.
- Visual field impairment
- Photopsia
- Diplopia
- Eye pain
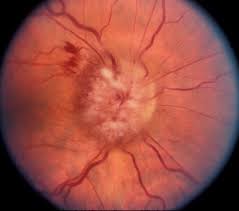
- Papilloedema
- CN VI and VII palsies
Diagnostic Criteria
Those patients with papilloedema
- Normal Neurological Examination
- Normal CSF composition
- Normal imaging ie., no signs of hydrocephalus
- Elevated Lumbar puncture opening pressures of >25cm in adults
The diagnosis can also be made in those patients without papilloedema but all the other findings above including unilateral or bilateral abducens nerve palsy.
Aetiology
The aetiology generally remains unknown however some of the proposed primary mechanisms include:
- Increased cerebral volume
- Increased CSF volume due to increased production and a resistance to outflow
- Obesity may raise intra-abdominal pressure increasing pleural and cardiac filling pressures and impeding venous return from the brain.
- Increased abdominal pressure, due to central obesity, also may limit the expansion of spinal CSF spaces
- Loss of cerebral autoregulation
- Increased cerebral venous pressure
Secondary causes of PTCS include:
- Disorders of the hypothalamic-pituitary-adrenal axes
- Cushing’s disease
- Addison’s disease
- Withdrawal from steroid use.
- Impaired sodium homeostasis, which can be an impairment of sodium and water excretion.
Conclusion
The greater the BMI and percentage of weight gain, the greater the chance of developing raised intracranial pressure. However a 5-15% increase in weight gain is all that is required for symptoms to appear. Thus small decreases ie., of this same magnitude are thought to decrease the symptoms. However there seems to be no correlation between the degree of weight loss and the reduction in intracranial pressure.
Something to think about.
References
- Andrews L et al. Idiopathic Intracranial Hypertension and Obesity. Horm Res Paediatr 2014;81:217-225.
- Kesler A et al. Idiopathic intracranial hypertension: risk of recurrences. Neurology. 2004;63:1737–1739.
- Kesler A et al. Do men with pseudomotor cerebri share the same characteristics as women? A retrospective review of 141 cases. J Neuroophthalmol. 2001;21:15–17.










This design is wicked! You definitely know how to keep a reader entertained.
Between your wit and your videos, I was almost moved to
start my own blog (well, almost…HaHa!) Fantastic job.
I really loved what you had to say, and more than that, how
you presented it. Too cool!