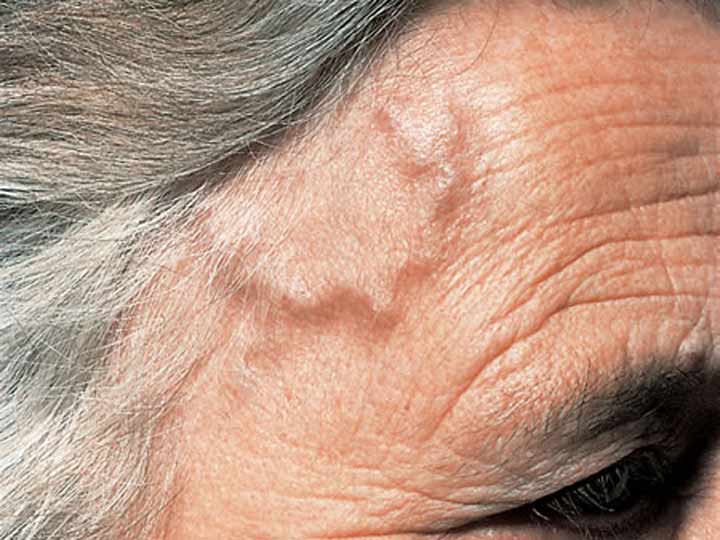
Temporal Arteritis also known as Giant Cell Arteritis, affects the medium and large arteries and is a vasculopathy. The greatest risk, if not treated, is irreversible loss of vision. It is a medical emergency.
CASE
A 79 year old woman has been sent in by her GP, complaining of unbearable, intractable headache for the past the past 10 weeks. She does not normally complain of headaches. The headache is occipito-frontalis in nature and over the forehead and both temporal regions. There is paravertebral pain along the cervical spine, but no vertebral pain. There has been no head strike of any sort.
The recent history has been one of the increasing headaches not controlled by simple paracetamol now requiring Panadeine Forte and Pregabalin. The headaches never totally recede, but return when the medication wears off.
Past Medical History includes hypertension, Meniere’s disease and hypercholesterolaemia. There is a history of a distal radial fracture, some months ago, secondary to a mechanical fall and for which the patient did not seek help for almost 1½ weeks whilst continuing her daily gardening. There were no other injuries at the time.
This is a fit lady who walks every day for two to three kilometres and maintains a large garden.
The patient has been seeing a GP in the practice, who does not usually look after her. The diagnosis has been cervical arthritic pain. Laser acupuncture has been used for a few weeks with some improvement in the right paravertebral muscles, but the headaches are still severe, reaching 10/10.
The patients’s normal GP, on return, has ordered an MRI of the brain which was normal. He had also ordered blood tests and these were essentially normal except for a ESR of 40. (Expected ESR for age is 79/2 = 40). BUTT the ESR was normal one year ago. Based on this story, the GP is concerned about temporal arteritis and has referred her to the Emergency Department.
When you see the patient she has a headache of 5/10, as she has recently taken her Panadeine Forte. There is no cervical tenderness, but there is discomfort at the vertex of the head and the occipital-frontalis muscle is tender. There is no pain over the temporal regions and no Temporal Artery can be felt. This potentially makes Temporal Arteritis less likely as a diagnosis.
Cranial nerve examination including visual acuity are all normal and there is nothing to see in the auditory canal. Examination of the upper and lower limbs is also normal. Pressures in the eye are also normal.
You pick up the phone and talk to the ophthalmology Registrar, to get an opinion. The registrar says, “I don’t think so. The ESR is raised but its okay for her age and she has no temporal artery pain as such. Send her home we can see her in Outpatients in a couple of weeks”.
The American College of Rheumatology has four criteria, which if present, requires the patient be offered a biopsy to confirm the diagnosis. These are:
- Age > 50
- New onset headache, or localised head pain
- Temporal artery pain to palpation or a reduced pulsation
- ESR > 50mm/hr ( it is usually measure in woman as (age + 10/2)
The patient has three of the four. What other explanation is there?
This is a woman who has never had headaches before, with a new severe headache and negative MRI brain. She is not a complainer. She tolerated a fractured distal radius for a week, whilst working in her garden. The headaches aren’t being controlled by analgesia.
Hmmm. It just doesn’t feel right! For those of you working for a few years, you know what I mean.
You speak to the medical registrar and she is admitted. She is started on Prednisolone 50mg daily for three days and booked for a Temporal Artery Biopsy, the next day. Later that evening, she tells you that the headache has improved significantly following the prednisolone.
The biopsy results come back at day 3: POSITIVE for Giant cell arteritis. She is commenced on 75mg of Prednisolone for 3 days, 50mg for a week and then 25mg for the next short time, until seen again.
This was a lucky case. BEWARE temporal arteritis, it can mimic other conditions.
HOW DO PATIENTS PRESENT?
- Constitutional Symptoms: Patients can present with a simple low grade fever and lethargy.
- Headache: Headache is the chief complaint and occurs in up to 2/3 of cases
- Headache Location: The headache is usually temporal, but may occur anywhere.
- Amaurosis Fugax: Abrupt, painless, monocular partial field loss must be investigated
- Painless Visual Loss: It occurs in about 20% of cases and is usually irreversible. It can be partial or complete, unilateral or bilateral. If there is no visual loss when glucocorticoids are commenced, there is virtually no chance of visual loss occurring. That is why early diagnosis and treatment is important. Most cases of visual loss in these patients is caused by anterior ischemic optic neuropathy and this is of the posterior ciliary artery which supplies the optic nerve and is a branch of the ophthalmic artery.
- Jaw Claudication: Fatigue of the muscles of mastication occurs rapidly when chewing
- Diplopia: It occurs in 5% of Gian Cell Arteritis. If there are any other symptoms, think of this.
INVESTIGATIONS
There are so many other investigations we can perform, however a simple ESR and CRP are very important to assist with the diagnosis. ESR can reach 100mm per hour. However, it does not have to be high and about 5% of the population have an ESR of < 40.
DIAGNOSIS
Diagnosis should not be based on symptoms only. The patient needs a temporal artery biopsy. A normal Temporal Artery biopsy does not exclude the disease however as ‘skip’ lesions can occur. If there is a negative biopsy on one side, the chance of a positive on the other is about 1%.
In patients that present with a more generalised headache and Temporal Arteritis cannot be excluded, bilateral biopsies are required.
SHOULD GLUCOCORTICOIDS BE COMMENCED BEFORE A BIOPSY?
Yes. The steroids do not affect the biopsy, as it takes up to a month to reduce the inflammation.
PEARLS NOT TO MISS THE DIAGNOSIS
- Think of it in any person over 50 yo who presents with a new headache.
- Women are more often affected than men
- It overlaps with Polymyalgia Rheumatica
- Think of it in any patient with diplopia, or amaurosis fugax
- Jaw Claudication(ie., pain on eating) occurs in 20% of patients with the disease.