A 50 year old man presents to the emergency department with shortness of breath and sharp chest pain for the previous 24 hours. There has been no trauma and the patient has no past medical history, on no medications and denies the use of any illicit drugs. This is his ECG: Please make a diagnosis and give an outline of the causes.
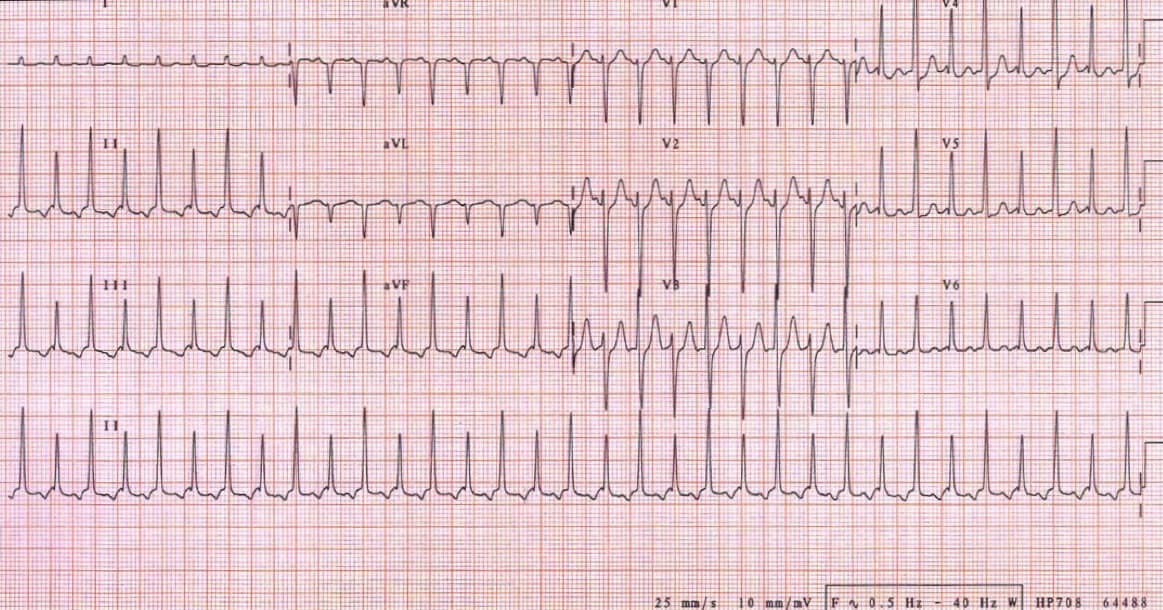
Using the ‘ECG in 20 Seconds’ method:
Rate: 25 x 6 = 150 bpm
Rhythm: It is hard to see P waves at this rate, however, I believe that there are P waves in V1 and V5 and II, so I will call this sinus rhythm
QRS: Narrow complexes, borderline left ventricular hypertrophy, with normal morphology(no delta wave), except that the height of the QRS alternates, between high and low. This is ELECTRICAL ALTERNANS.
Axis: Normal
ST-T: There is no evidence of ST elevation, but there is some ST depression evident in lead V4, which is probably rate related. The T waves look a little peaked in V3 and there is T wave inversion in the inferior leads.
PR/QT: PR interval is fine, although the QT interval is prolonged.
The diagnosis is a sinus tachycardia with electrical alternans.
The causes of alternans are several but mainly fall into three categories:
1. Repolarisation: This involves the ST segments and the T wave.
T wave alternans is reported in long QT syndrome(precursor to Torsades) and in electrolyte abnormalities(hypo-Ca,K,Mg). It is also associated with cardiomyopathy or acute pulmonary embolism.
ST alternans is associated with changes in ST segment during ischaemia and is associated with acute myocardial infarction.
2. Conduction alternans: This is the result of a change in impulse propagation
It is seen in myocardial infarction, atrial fibrillation and Wolf Parkinson White syndrome and pulmonary embolism. In the setting of a narrow QRS tachycardia, it may be an orthodromic atrioventricular re-entry tachycardia.
3. Cardiac motion: This is the result of abnormal movement of the heart.
It can be caused by pericardial effusion and hypertrophic cardiomyopathy.
In this patient at 50 years of age and with no previous history and the atypical nature of the pain a pericardial effusion is a probable cause, however, the complexes are large, not dampened by fluid in the sack. Could it be ischaemic? Absolutely. Could it be a repolarisation issue caused by long QT? It could be.
Given that it is a QRS alternans and the normal sized complexes, I would have as my initial diagnosis, pulmonary embolism, followed by myocardial infarction, followed by pericardial effusion.
Even though it is 3rd on my differentials, I can quickly look at the pericardium, by doing a rapid echo with the emergency department ultrasound machine. If this is normal, then the workup continues for a clot or ischaemia.










continuously i used to read smaller articles which also clear
their motive, and that is also happening with this piece of writing which I am
reading at this place.
Hello there, There’s no doubt that your blog could possibly be having browser compatibility issues.
Whenever I take a look at your blog in Safari, it looks fine
however, when opening in I.E., it has some overlapping issues.
I merely wanted to give you a quick heads up!
Aside from that, great website!
I like looking at and I think this website got some truly useful
stuff on it!
Feel free to visit my website :: https://groups.google.com/g/cannabidoil-reviews/c/1DGiKWNIb2M
Informative article, exactly what I was looking for.
Also visit my web site https://www.tumblr.com/blog/keonicbd-review (http://www.tumblr.com)
Wow, that’s what I was looking for, what a stuff! present here at this webpage, thanks
admin of this web site.
Here is my website :: https://yclas380.00web.net/market/keoni-cbd-support-health-today.html (yclas380.00web.net)
Great post. I was checking constantly this blog and
I am impressed! Very useful information specifically the last
part 🙂 I care for such information much. I was looking for this
certain information for a very long time. Thank you and good luck.
Have a look at my web-site :: https://penzu.com/p/4c89d665 (penzu.com)
Keep functioning ,fantastic job!
Also visit my homepage :: https://justpaste.it/85tci, https://justpaste.it,
It’s the best time to make a few plans for the future and it is time to be
happy. I have learn this submit and if I may just I wish to recommend
you some fascinating issues or advice. Perhaps you could write subsequent articles
regarding this article. I desire to read even more issues approximately it!
My web blog :: https://kit.co/claudialade/keoni-cbd-gummies (Rudolf)
I conceive you have observed some very interesting points, appreciate it for the post.
My website … https://justpaste.it/85uyf
Great post. I was checking continuously this blog and I am impressed!
Very useful information specially the last part 🙂 I care for such information much.
I was seeking this certain information for a long time.
Thank you and good luck.
My website – http://recampus.ning.com/profiles/blogs/keoni-cbd-support-health-today (recampus.ning.com)
Aw, this was an extremely good post. Finding the time and actual effort to produce a superb article…
but what can I say… I procrastinate a whole lot and don’t seem to get anything done.
Feel free to surf to my page – http://keoni-cbdreview.ampblogs.com/Keep-Health-Problems-Away-With-Keoni-Hemp-Oil–39472764 (keoni-cbdreview.ampblogs.com)
I think this internet site has got some very wonderful info
for everyone :D.
Also visit my site … https://www.tumblr.com/blog/keoni-cbdreview
Wow, that’s what I was seeking for, what a data! present
here at this blog, thanks admin of this web site.
my website; http://keonicbd-review.ampblogs.com/Keoni-CBD-Support-Health-Today–39472010 [keonicbd-review.ampblogs.com]
It’s perfect time to make a few plans for the long
run and it’s time to be happy. I have learn this publish and if
I may just I desire to suggest you some interesting issues or advice.
Maybe you can write subsequent articles referring to this article.
I desire to read even more issues approximately it!
Feel free to visit my web-site https://keoni-cbdreview.mystrikingly.com/ (Delia)
Unquestionably believe that which you stated.
Your favorite justification appeared to be on the internet the easiest thing to be aware of.
I say to you, I definitely get irked while people think about worries that they plainly don’t know about.
You managed to hit the nail upon the top and also defined out the whole thing without having side effect , people could
take a signal. Will likely be back to get more. Thanks
You have made some really good points there. I checked on the web to find out more about the issue and found
most individuals will go along with your views on this website.
Also visit my web blog – https://sites.google.com/view/keonicbd-review/home – sites.google.com,
Great post. I was checking constantly this blog and I am impressed!
Very useful information particularly the final
part 🙂 I take care of such information much.
I was seeking this certain info for a very long time. Thank you and good luck.
Also visit my homepage – https://docs.google.com/presentation/d/e/2PACX-1vSihxVkBBVdWV2_22g6-WUKFz64OxMHYt7y-2d_RhcJIT9O8Wr_jrBi1rTnGVoLHztbvv2OFvvEuRkw/pub?start=false&loop=false&delayms=3000 – docs.google.com –