Our obsession with adrenaline continues. We want to prove it works. It must! If it doesn’t what do we have? We’ve been running arrests in this way for the last 50 odd years. If they took adrenaline away, what’s left?
Our obsession with adrenaline continues. We want to prove it works. It must! If it doesn’t what do we have? We’ve been running arrests in this way for the last 50 odd years. If they took adrenaline away, what’s left?
I ran a resus two days ago on a patient with refractory pulseless VT. When I looked up at the end of the resus, we must have given about 20mg or more, of adrenaline. The outcome was still not good.
We know that in cardiac arrest only two of the weapons we have work. They are chest compressions and defibrillation. Airway and adrenaline don’t add much. Does adrenaline actually add anything?
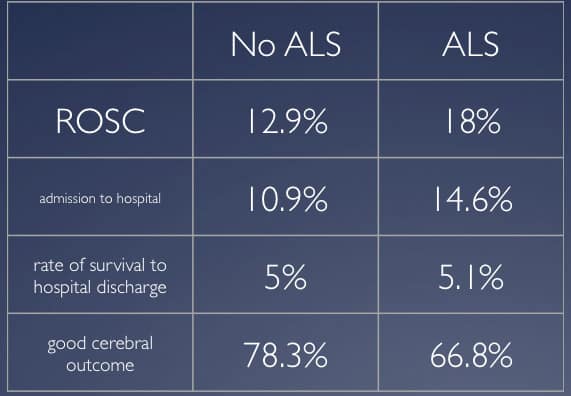 The landmark OPALS study by Steil et al NEJM 2004;351:647-656, looked at the effect of adding advanced life support(ACLS) to the rate of out of hospital survival, following cardiac arrest. ACLS is really about airway and adrenaline. The results are shown in the table. Those patients receiving ACLS had a higher rate of return of spontaneous circulation(ROSC) and a higher rate of admission to hospital. However, the rate of survival to hospital discharge, which is what we really care about, was no different between the two groups. In fact, those receiving ACLS had a worst cerebral outcome.
The landmark OPALS study by Steil et al NEJM 2004;351:647-656, looked at the effect of adding advanced life support(ACLS) to the rate of out of hospital survival, following cardiac arrest. ACLS is really about airway and adrenaline. The results are shown in the table. Those patients receiving ACLS had a higher rate of return of spontaneous circulation(ROSC) and a higher rate of admission to hospital. However, the rate of survival to hospital discharge, which is what we really care about, was no different between the two groups. In fact, those receiving ACLS had a worst cerebral outcome.
Here are some recent papers.
STUDY 1
Jacobs et al. Effect of Adrenaline on survival in out of hospital cardiac arrest: A randomised double blind controlled trial. Resuscitation 2011, Sept;82:1138
534 adults randomised to either 1ml adrenaline(1:1000) or 1 ml normal saline, every 3 minutes.
Setting: Out of hospital cardiac arrest.
The patients receiving adrenaline:
- had significantly higher ROSC in the pre-hospital setting (23.5% vs 8.4%)
- had statistically significant, higher admission rate to hospital from the emergency department(25.4% vs 13%)
BUT … the rate of survival to discharge did not differ significantly between the two groups.
The study was underpowered.
STUDY 2
Hagihara et al Prehospital epinephrine use and survival among patients with out of hospital cardiac arrest JAMA 2012 Mar 21;307:1161
This was a prospective observational study of 417,188 out of hospital cardiac arrests in Japan.
The rate of return of spontaneous circulation to hospital arrival was higher in the adrenaline group. There was no standardisation of hospital care in this study. The rate of survival at one month, in those receiving adrenaline was significantly lower. Not the same, but adrenaline made it worst.
So what’s the answer?
I recently spoke on this at the ACEM Annual Scientific Meeting. I’m not sure that the current guidelines that we have, are the ‘golden bullet’, but we don’t have anything else currently. There are some very smart people out there working on it right now.
What can we do? We can use the adrenaline to ensure that people get to us, at the hospital. It is then our responsibility to ensure that we have the skills and knowledge in our resuscitation efforts, to apply the rest of the resuscitation guidelines to their maximum. We need to know about airway and hyperventilation, adequate chest compressions in terms of rate, depth and cycle, minimum interference with compressions and the need to ensure we know when there is output, so we don’t give adrenaline and create a massive after load. We need to apply cooling and any other efforts that may make a difference. This is all about training and it’s not easy. It takes weeks of looking at the literature and understanding where there is some evidence and where there isn’t.
The reality is, that there’s not much evidence out there, but it’s all we have. Make sure you know how to do it.
“The knowledge you take into your shift does matter!” Peter Kas